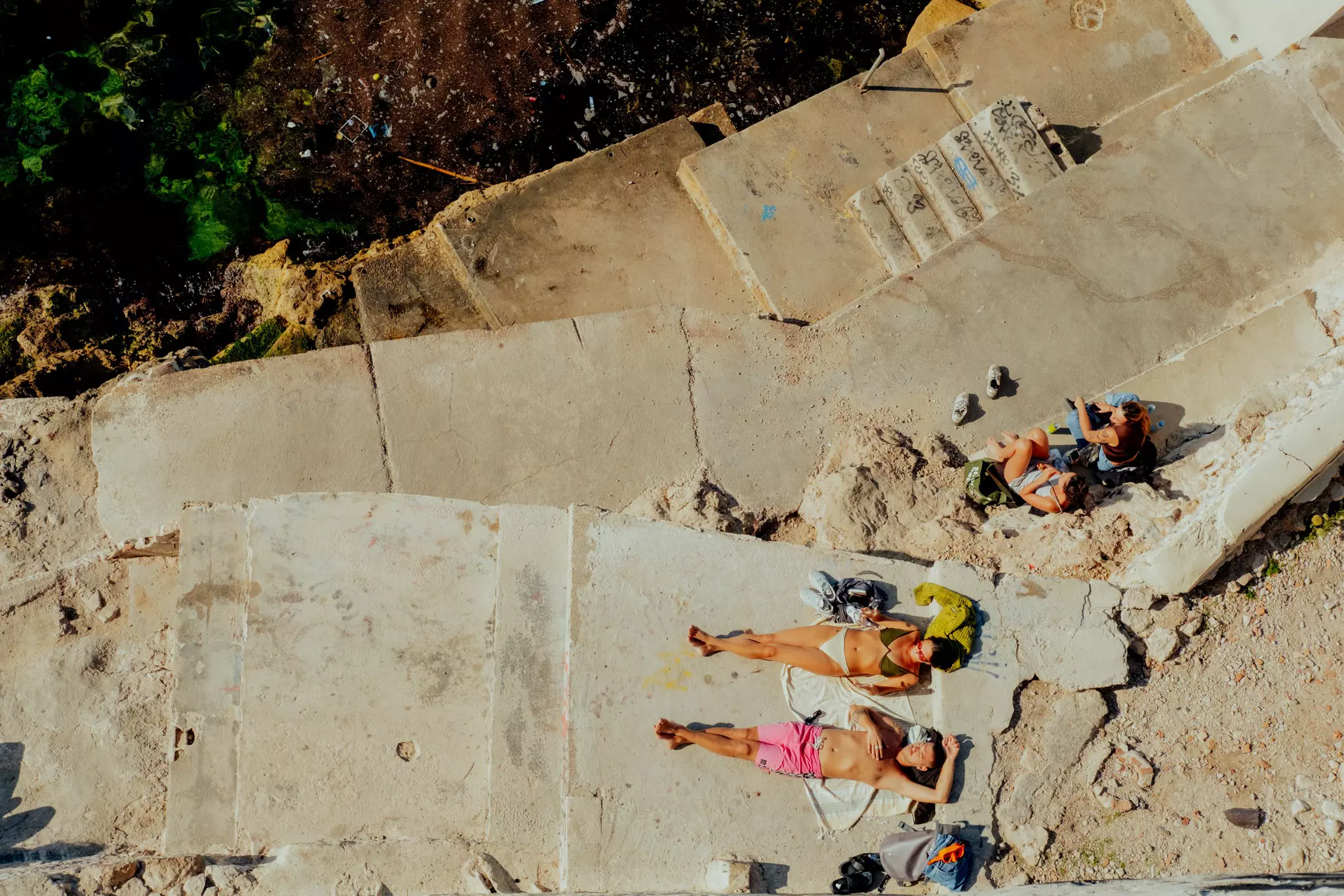Sri Lanka

Athikhom Saengchai/Shutterstock

Why visit Sri Lanka
Endless beaches, timeless ruins, welcoming people, oodles of elephants, rolling surf, cheap prices, fun trains, famous tea and flavorful food make Sri Lanka irresistible.
Lonely planet’s trusted travel insurance provider
Dreaming of Sri Lanka? Protect your trip
Travel with confidence. Protect your trip and your wallet.
We don’t represent World Nomads, we receive a fee from quotes using this link. This is not a recommendation to buy travel insurance.
Take your Sri Lanka trip with Lonely Planet Journeys
Pick one of our ready-to-book trips or fully customize your own with help from our local experts.
bookable trip
Snapshots of Sri Lanka: 15-day Cultural Cross-Country Odyssey
15 days / 14 nights
highlights
- 1 Visiting Sigirya’s hidden gems and iconic landmarks, including its famous, frescoed rock fortress
- 2 Embarking on a scenic train adventure that will lead you through Sri Lanka’s diverse landscapes
- 3 Snorkeling Trincomalee's crystal clear waters to uncover diverse species of fish and sea turtles
from $4,050
per person


Explore more trips
Explore more trips

14 days / 13 nights
Signature Sri Lanka: City, Coast, and Wildlife Corridors in 14 Days
FROM $2,925
per person
Top places to visit in Sri Lanka
Discover the best attractions in Sri Lanka from must-see sights to unexpected hidden gems.
Travel Guides
Sri Lanka travel tips from Lonely Planet experts
Find practical guidance from our team of contributors around the world who bring their decades of first-hand travel experience to your next trip.
Best Things to Do
Sri Lanka is a nature lover’s dream. Here’s how to get the most out of its gorgeous waterfalls, lush rainforests, teeming coral reefs and surf-ready waves.
Read full article
Best Time to Visit
Whether you want to surf, hike or spot elephants, Sri Lanka delivers. Here’s our season-by-season guide.
Read full article
Things to Know
Follow these 23 tips on etiquette and customs in Sri Lanka and your visit to this pearl in the Indian Ocean will be both full and respectful.
Read full article
Transportation
Our guide to transportation can help you plan the best way for your travels around Sri Lanka.
Read full article
Visa Requirements
If you’re planning a trip to Sri Lanka, chances are you’ll need a visa when you arrive. Here’s all you need to know about how to get one.
Read full article
Best Road Trips
Hire a car and driver or rent a motorcycle and explore the best of Sri Lanka with these road trip routes.
Read full article
Traveling with Kids
Whether you're traveling with toddlers or teenagers, here's where to stay and what to do for an unforgettable family adventure in Sri Lanka.
Read full article
Best Places to Visit
This beguiling island nation is packed with beautiful beaches, culture-packed cities and lush mountains. Here are some top Sri Lankan places to visit.
Read full article
Get Connected
Sri Lanka is the perfect Indian Ocean getaway, and your cell phone is a handy tool for exploring. Here's what you need to know about getting connected.
Read full article
in partnership with getyourguide