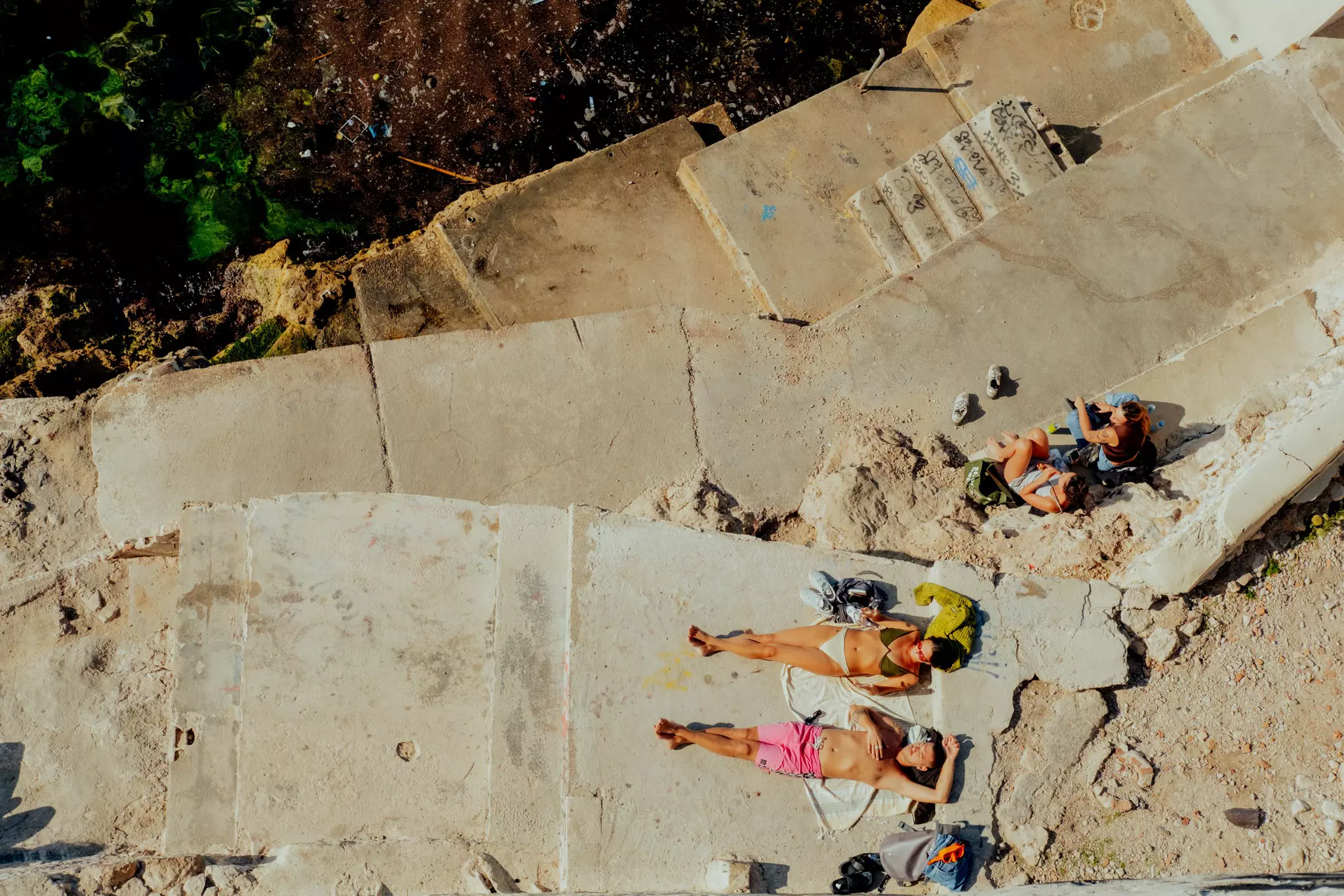Egypt
Egypt welcomes you with its mighty Nile and magnificent monuments, the beguiling desert and lush delta, and with its long past and welcoming, story-loving people.

Getty Images/iStockphoto
- Monica Gerges|Feb 18, 2026How to get your cell phone connected in Egypt: eSIMs, wi-fi and mobile networks
- Shoroq Galal|Feb 10, 2026A guide to outdoor adventures in Egypt
- Lonely Planet Editors|Dec 22, 2025The 9 best places for diving and snorkeling in Egypt’s Red Sea
- Monica Gerges|Dec 18, 202514 of the best things to do in Egypt



Dreaming of Egypt? Protect your trip
Travel with confidence. Protect your trip and your wallet.
We don’t represent World Nomads, we receive a fee from quotes using this link. This is not a recommendation to buy travel insurance.
Take your Egypt trip with Lonely Planet Journeys
Pick one of our ready-to-book trips or fully customize your own with help from our local experts.
bookable trip
10 Days in Egypt: Nile Cruise of Ancient Wonders
highlights
- 1 Cruising down the Nile on a four-night odyssey from Luxor to Aswan
- 2 Riding a camel around the world-famous Pyramids of Giza
- 3 Harnessing the knowledge of the ancient world at the Library of Alexandria
from $3,710
per person


Top places to visit in Egypt
Discover the best attractions in Egypt from must-see sights to unexpected hidden gems.
Travel Guides
Egypt travel tips from Lonely Planet experts
Find practical guidance from our team of contributors around the world who bring their decades of first-hand travel experience to your next trip.
Best Things to Do
You might visit Egypt for the history, the adventure, the beaches or even just the pyramids - when it comes to things to do, you are spoiled for choice.
Read full article
Best Time to Visit
With tombs, pyramids and towering temples, Egypt brings out the explorer in all of us. This handy month-by-month guide shows the best time to visit Egypt.
Read full article
Things to Know
From getting around to staying safe to minding your etiquette, here are our top tips for visiting Egypt.
Read full article
Transportation
From overnight trains to cruise boats on the Nile, here are the best ways to travel around in Egypt.
Read full article
Visa Requirements
Before you set off on your Egypt adventure, check this handy guide to find out all the Egyptian visa information you need for your trip.
Read full article
Best Road Trips
Experience the best of Egypt with these spectacular road trip routes.
Read full article
Money and Costs
Don't think a small budget will restrict your Egyptian adventure. With our top tips, you can explore the whole country without breaking the bank.
Read full article
Traveling with Kids
Egypt can be a challenging destination to visit, but the country is a treasure trove of activities for families. Here's how to visit Egypt with kids.
Read full article
Best Places to Visit
From Tutankhamun's tomb to the Karnak Temple Complex, the structures in this region are filled with fascinating history.
Read full article
Get Connected
Stay connected on your travels in Egypt with this guide to cell coverage, networks and wi-fi.
Read full article
Get a book. Get inspired. Get exploring.
in partnership with getyourguide